VIVO Pathophysiology
Cholecystokinin
Cholecystokinin plays a key role in facilitating digestion within the small intestine. It is secreted from mucosal epithelial cells in the first segment of the small intestine (duodenum), and stimulates delivery into the small intestine of digestive enzymes from the pancreas and bile from the gallbladder. Cholecystokinin is also produced by neurons in the enteric nervous system, and is widely and abundantly distributed in the brain.
Structure of Cholecystokinin and Its Receptors
As mentioned previously, cholecystokinin and gastrin are highly similar peptides. Like gastrin, cholecystokinin is a linear peptide that is synthesized as a preprohormone, then proteolytically cleaved to generate a family of peptides having the same carboxy ends. Full biologic activity is retained in CCK-8 (8 amino acids), but peptides of 33, 38 and 59 amino acids are also produced. In all of these CCK peptides, the tyrosine seven residues from the end is sulfated, which is necessary for activity.
Two receptors that bind cholecystokinin have been identified. The CCKA receptor is found abundantly on pancreatic acinar cells. The CCKB receptor, which also functions as the gastrin receptor, is the predominant form in brain and stomach. Both receptors are have seven transmembrane domains typical of G protein-coupled receptors.
Control and Physiologic Effects of Cholecystokinin
 Foodstuffs flowing into the small intestine consist mostly of large macromolecules (proteins, polysaccharides and triglyceride) that must be digested into small molecules (amino acids, monosaccharides, fatty acids) in order to be absorbed. Digestive enzymes from the pancreas and bile salts from the liver (which are stored in the gallbladder) are critical for such digestion. Cholecystokinin is the principle stimulus for delivery of pancreatic enzymes and bile into the small intestine.
Foodstuffs flowing into the small intestine consist mostly of large macromolecules (proteins, polysaccharides and triglyceride) that must be digested into small molecules (amino acids, monosaccharides, fatty acids) in order to be absorbed. Digestive enzymes from the pancreas and bile salts from the liver (which are stored in the gallbladder) are critical for such digestion. Cholecystokinin is the principle stimulus for delivery of pancreatic enzymes and bile into the small intestine.
The most potent stimuli for secretion of cholecystokinin are the presence of partially-digested fats and proteins in the lumen of the duodenum (a particularly potent stimulus is pictured above). An elevation in blood concentration of cholecystokinin has two major effects that facilitate digestion:
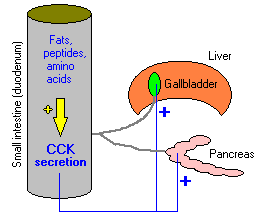
- Release of digestive enzymes from the pancreas into the duodenum. Older literature refers to cholecystokinin as pancreozymin, a term coined to describe this effect.
- Contraction of the gallbladder to deliver bile into the duodenum. The name cholecystokinin (to "move the gallbladder") was given to describe this effect. Cholecystokinin is also known to stimulate secretion of bile salts into the biliary system.
Pancreatic enzymes and bile flow through ducts into the duodenum, leading to digestion and absorption of the very molecules that stimulate cholecystokinin secretion. Thus, when absorption is completed, cholecystokinin secretion ceases.
Injection of cholecystokinin into the ventricles of the brain induces satiety (lack of hunger) in laboratory animals. In view of its pattern of secretion relative to feeding, it would make physiologic sense that this hormone might participate in control of food intake. However, recent experiments suggest that cholecystokinin is at best a minor player in regulation of food intake.
In addition to its synthesis in small intestinal epithelial cells, cholecystokinin has been clearly demonstrated in neurons within the wall of the intestine and in many areas of the brain. It seems, in fact, to be the most abundant neuropeptide in the central nervous system. Secretion of cholecystokinin from neurons appears to modulate the activity of other hormones and neuropeptides, but it seems safe to say the understanding its role in function of the brain is rudimentary at best.
Disease States
Diseases resulting from excessive or deficient secretion of cholecystokinin are rare. Cholecystokinin deficiency has been described in humans as part of autoimmune polyglandular syndrome, and was manifest as a malabsorption syndrome clinically similar to pancreatic exocrine insufficiency. Additionally, there is mounting evidence that aberrations in expression of cholecystokinin or its receptor within the human brain may play a part in the pathogenesis of certain types of anxiety and schizophrenia. Clearly, a much better understanding of the role of cholecystokinin in brain function is required.
Send comments to Richard.Bowen@colostate.edu

